 Our knees handle an immense amount of stress each day as we run and walk, and if you develop pain or discomfort in your knees, it can make movement downright difficult. And while knee replacement operations are available for severe knee joint deterioration, you may be able to avoid surgery and alleviate symptoms if you know how to treat chronic knee pain when it first develops. In today’s blog, we share four tips for overcoming chronic knee pain.
Our knees handle an immense amount of stress each day as we run and walk, and if you develop pain or discomfort in your knees, it can make movement downright difficult. And while knee replacement operations are available for severe knee joint deterioration, you may be able to avoid surgery and alleviate symptoms if you know how to treat chronic knee pain when it first develops. In today’s blog, we share four tips for overcoming chronic knee pain.
How To Treat Chronic Knee Pain
Here’s a closer look at some of the most commonly recommended treatments for chronic knee pain, and why they may be helpful for your joint discomfort.
1. Movement – It may sound odd that we’re recommending putting more stress on an area of your body that’s hurting, but movement and exercise can be exactly what your knee needs. Movement helps to push healthy blood to and from the area, and it strengthens nearby structures to make it easier for the knee to handle stress. You just want to be smart in what types of movement you pursue. Low-impact movements and exercises are preferred to a high-impact exercise like running, so start walking, swimming or cycling more often, and your knee should become stronger.
2. Weight Loss – Another way to help lessen knee pain is to find ways to take stress off the area, and one such way is to lose weight. Your knees handle the stress of your body when you’re standing and moving, so the less you weigh, the less pressure they’ll be under. Even losing just a few pounds can take a large load off your knee, so dieting and exercising can really help to alleviate chronic knee pain.
3. Physical Therapy – You can also target the knee and surrounding tissues specifically with the help of physical therapy. In Minnesota, you don’t need a referral in order to seek assistance for a medical issue with a physical therapist, so you can go directly to the source if you’d like to see if PT can help. They’ll conduct a baseline assessment, have you perform some in-person exercises and set you up with an individualized therapy routine that you can perform from the comfort of your home to strengthen your knee.
4. See A Pain Specialist – Knee pain is one of Dr. Cohn’s specialties, and he’d be more than happy to conduct a comprehensive examination of your knee and the connected systems to understand the full scope of your knee issue. Not only can he walk you through some non-operative treatment methods, but he can explain why these techniques should help provide relief. When you have a clearer understanding of your issue and the ways to treat it, you’re more likely to have success pursuing these treatment options.
So if you are dealing with lingering knee pain that is preventing you from enjoying certain aspects of life, consider the above tips or take a minute to set up an appointment with a pain management specialist like Dr. Cohn. We can help you regain your independence and improve your quality of life by reducing or eliminating your knee pain. For more inforamtion, give his office a call today at (952) 738-4580.
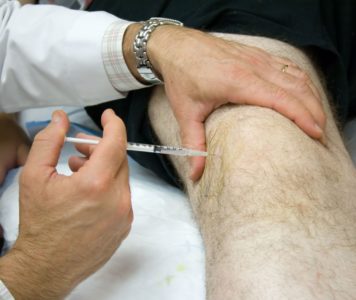 In general, the development of hyaluronate sodium for knee osteoarthritis dates back to the early to mid 1990’s. The full mechanism on how these compounds work has not been fully understood, but it is believed that they stimulate the cells in the joints to produce joint fluid and thus provide lubrication and cushioning within the joint. In the United States, these compounds have only been FDA approved for the use in the knee joint, but around the world they have been used successfully in a number of joints including shoulders, hands, hips and feet.
In general, the development of hyaluronate sodium for knee osteoarthritis dates back to the early to mid 1990’s. The full mechanism on how these compounds work has not been fully understood, but it is believed that they stimulate the cells in the joints to produce joint fluid and thus provide lubrication and cushioning within the joint. In the United States, these compounds have only been FDA approved for the use in the knee joint, but around the world they have been used successfully in a number of joints including shoulders, hands, hips and feet.

