 The physical pain of a chronic pain condition gets most of the attention, but a pain issue affects you in more than just a physical manner. There is also a significant mental and emotional side of chronic pain, and if you aren’t careful in how you treat the problem, you may find that the issue never fully resolves. In today’s blog, we take a look at some ways to tackle these three sides of a chronic pain problem.
The physical pain of a chronic pain condition gets most of the attention, but a pain issue affects you in more than just a physical manner. There is also a significant mental and emotional side of chronic pain, and if you aren’t careful in how you treat the problem, you may find that the issue never fully resolves. In today’s blog, we take a look at some ways to tackle these three sides of a chronic pain problem.
Managing The Physical Side Of Chronic Pain
Let’s start by looking at the physical ways you can fight back against your chronic pain condition. These are some of the most common treatments that will be recommended from your pain management specialist. Odds are they suggest a combination of some of the following techniques:
- Daily exercise
- Controlled stretching
- Physical therapy
- Posture improvements
- Weight loss
All of these techniques serve to make you physically stronger or make it easier for your body to handle the stress that you are putting on it. Because chronic pain is oftentimes tied to a stability issue or problematic inflammation, working to improving your body’s functional performance through physical activity and exertion and be extremely beneficial.
Managing The Mental Side Of Chronic Pain
A chronic pain condition can also put a significant burden on your mental health, so it’s important that you don’t ignore your mental health while you’re pursuing some of the physical treatments listed above. Chronic pain can leave you feeling worried and anxious, so you’ll want to make sure that you are stimulating your brain and working to appropriately frame your chronic pain condition in your mind. For example, don’t just lay in bed all day and hope that pain goes away. Find ways to stimulate your brain and take your mind off chronic pain. Pursuing mentally stimulating activities can lead to the production of hormones that can help drown out pain signals.
It’s also important that you have the right mindset when it comes to your chronic pain condition. It can be easy to catastrophize your pain condition or always view things with a “glass half empty” perspective. You can’t always control your pain, but there are certain aspects you can control, and if you put your time and effort into the aspects of your condition that you can control (like diet, exercise, mental stimulation), you can take solace in knowing you are doing what you need to do to fight back against chronic pain. Try not to focus on the uncontrollable and reframe how you approach your care, and you’ll find that you have more peace over your condition, which can actually help you overcome your pain!
Managing The Emotional Side Of Chronic Pain
Finally, chronic pain can also be very emotionally draining. If you’ve had your pain condition for a while, odds are you’ve had to cancel plans to stop pursuing certain activities you love because of your pain, and that can really wear on a person’s emotions. Similar to the above point on how you need to pursue activities that are mentally stimulating and rewarding, you need to also throw yourself into activities that are emotionally rewarding. Have a friend over for dinner, go for a walk with your sister, call your friend who moved across the country, etc.
You can also find emotionally rewarding activities that don’t depend on other people. Force yourself to go see that new movie, volunteer to walk a dog at the adoption shelter every Friday, or simply curl up with a new book. Chronic pain can be isolating and emotionally draining, so you also want to make sure that you are finding ways to add a little joy to your life. When you’re happier and emotionally balanced, it will be much easier to manage the ups and downs of a pain condition.
If you need help with any of these aspects, or your want to create an individualized care plan for your pain issue, reach out to Dr. Cohn and his team today at (952) 738-4580.
 New research from the University of Arizona Health Sciences and published in the journal PAIN found that nearly five million Americans experienced the co-occurrence of chronic pain and a mental health condition like anxiety or depression, leading to functional limitations in their daily life.
New research from the University of Arizona Health Sciences and published in the journal PAIN found that nearly five million Americans experienced the co-occurrence of chronic pain and a mental health condition like anxiety or depression, leading to functional limitations in their daily life.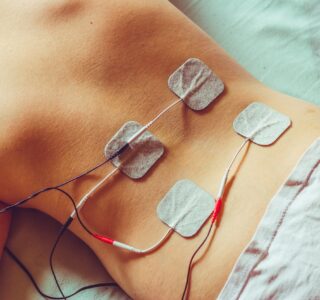 We always have our ear to the ground when it comes to learning about new potential forms of treatment for chronic pain, and one such treatment that is making waves in the pain care community is called scrambler therapy. But what is scrambler therapy, and could it really help you get control over your chronic pain condition? We take a closer look at the treatment in today’s blog.
We always have our ear to the ground when it comes to learning about new potential forms of treatment for chronic pain, and one such treatment that is making waves in the pain care community is called scrambler therapy. But what is scrambler therapy, and could it really help you get control over your chronic pain condition? We take a closer look at the treatment in today’s blog. Chronic pain affects tens of millions of Americans every day, and while everyone is going through their own individual battle, many of them are dealing with discomfort in similar locations. But what are some of the most common locations for chronic pain to develop, and why are these the most popular spots? In today’s blog, we take a closer look at five of the most common locations in your body for a chronic pain issue to develop.
Chronic pain affects tens of millions of Americans every day, and while everyone is going through their own individual battle, many of them are dealing with discomfort in similar locations. But what are some of the most common locations for chronic pain to develop, and why are these the most popular spots? In today’s blog, we take a closer look at five of the most common locations in your body for a chronic pain issue to develop. Back pain is incredibly common, but as we’ve said on the blog numerous times in the past, this doesn’t mean that back pain is normal. If you’re dealing with back pain, it’s imperative that you work to figure out the underlying cause so that treatment can begin. If you recently fell and injured your back, it will be easier to pinpoint your source of pain, but if back pain seems to develop out of nowhere, it may be harder to figure out what’s causing your discomfort.
Back pain is incredibly common, but as we’ve said on the blog numerous times in the past, this doesn’t mean that back pain is normal. If you’re dealing with back pain, it’s imperative that you work to figure out the underlying cause so that treatment can begin. If you recently fell and injured your back, it will be easier to pinpoint your source of pain, but if back pain seems to develop out of nowhere, it may be harder to figure out what’s causing your discomfort.